Veterinary Topics
INDEX OF TOPICS IN THIS SECTION:-
Allergic skin disease explained
Osteoarthitis
Allergens and allergic dermatitis
Danger for Hedgehogs
Animal Autism?
Dog Walking Etiquette
Signs of Pain in Pets
Blue green algae warning
Hot weather advice
Dog Breeds at risk of over heating
Sunscreen advice
Yellow Dog UK
Glaucoma
Stress
Colour codes on Guide Dog Harness
Baby Wild Birds
Lilies are poisonous
Potential poisons for dogs (including link to poisonous plants)
Bunny Dentist
Signs of unwellness in rabbits
Rabbit health information
Horse manure risk to dogs
Chocolate poisoning
Babesiosis and ticks
Tick alert
Alabama rot
Jerky treat risk
Cancer therapy
Dental disease
Slugs risk
Allergic skin disease
Dog faeces risk to livestock
Scroll down below to your topic of choice
Allergic Skin Disease explained
Watch a 3D video explaining canine allergic skin disease
Osteoarthritis "Just getting older?"
Many dogs suffer in silence with what is often referred to as "just getting older and slower". Using this check list you could identify if your best friend could benefit from the multitude of treatment options to allow a more active and happier life.
CONTACT THE SURGERY IF YOU CAN ANSWER YES TO THE QUESTIONS BELOW

THINK CATS AS WELL
It is estimated that 80% of elderly cats have osteoarthritis but do not manifest it like dogs. Instead of presenting lame they often show signs of poor grooming, becoming more grumpy, sleeping more, not jumping up to heights and reduced appetite. These cats can be helped by providing pain relief which will enrich their lives.
Ring to discuss if you are worried your feline friend is suffering from any of these.
NO THEY ARE NOT "JUST GETTING OLD"
Allergens and allergic dermatitis



Danger for Hedgehogs

Animal Autism?
This was an interesting article in FOCUS magazine

Dog Walking Etiquette


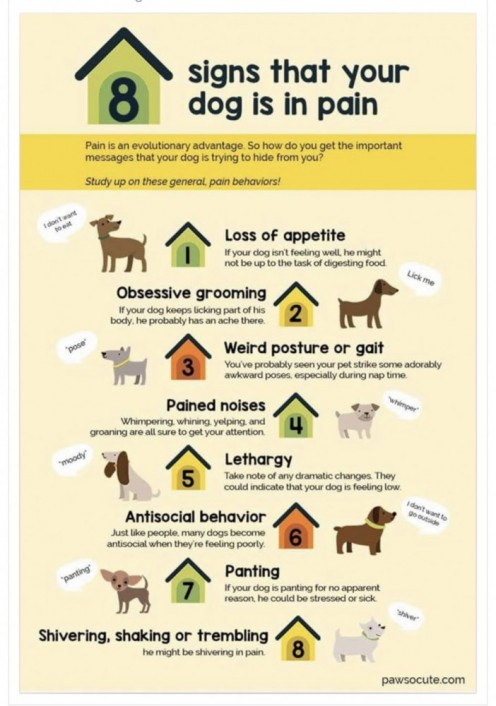
Signs of Pain in Pets

BLUE GREEN ALGAE WARNING
The recent warm weather has increased the risk of blue green algae poisoning. Blue green algae are cyanobacteria that proliferate in warm weather as a green, blue green or brown slime or scum on ponds and slow moving water. Some varieties produce potent toxins which can cause severe illness and death in dogs. Dogs can be poisoned by drinking contaminated water, or even licking their feet or coat after walking through infected water. Most parks will put notices up warning owners that levels are high and to keep dogs out of the water. Some strains are not harmful but it is impossible to tell them apart.
Signs include vomiting and diarrhoea, weakness, breathing problems, drooling, seizures, blood in faeces, coma and in some cases death. Progression can be rapid. If animals recover after treatment then long term issues are rare. Treatment involves fluid therapy on hospitalisation, along with supportive therapy with medication, oxygen and antiseizure medication if indicated.
Prevention is best, by keeping dogs away from ponds and slow moving fresh water when the weather is so warm, especially if there is a scum present, and it is important to check for warning notices.

ADVICE FOR HOT WEATHER RISKS


DOG BREEDS AT RISK OF OVER HEATING

SUNSCREEN ADVICE

YELLOW DOG UK
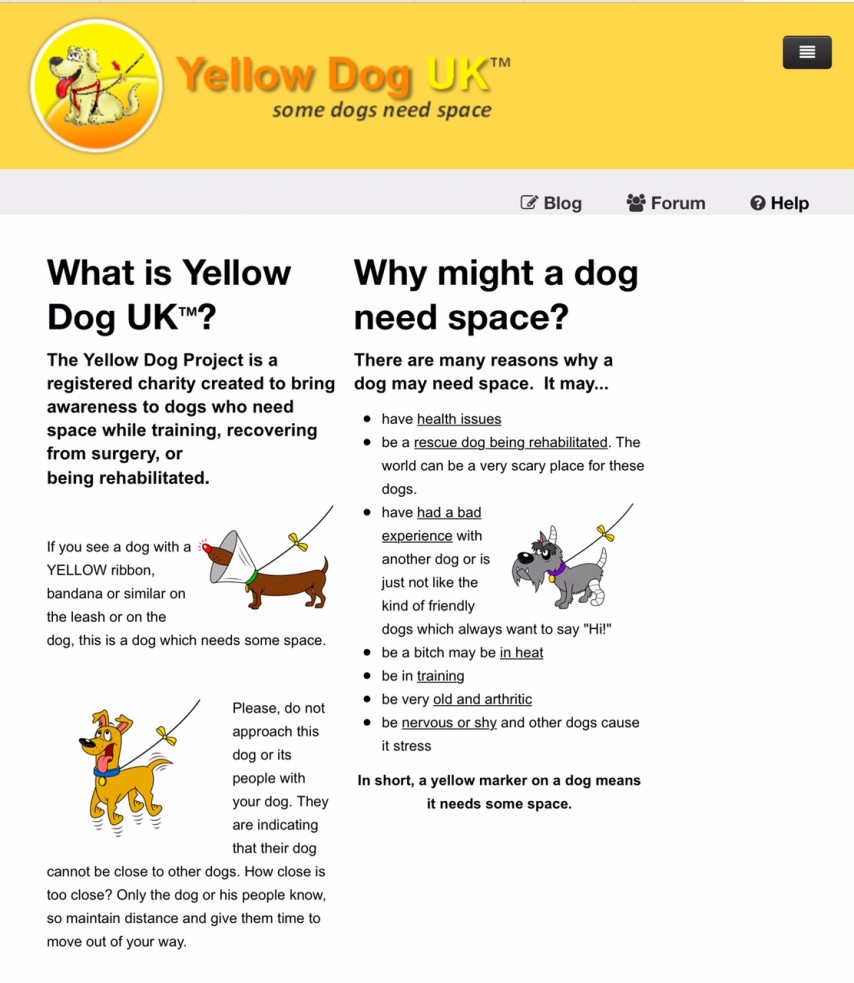
VISIT WWW.YELLOWDOGUK.CO.UK
GLAUCOMA
Glaucoma is an increase in the pressure inside the eye. There are various causes and some breeds (see below) are genetically predisposed to developing glaucoma. The condition is painful and when left unchecked can lead to permanent blindness. In the early stages it can be difficult to see any changes just looking at the eyes, and this is where measuring the intra ocular pressure (IOP), using an instrument called a tonometer, helps.
Making such measurements may be indicated in cases of Red eye, Head trauma, Eye trauma, Elderly dogs and at susceptible breeds annual check ups.
Susceptible Breeds:-
Afghan, Akita, Alaskan Malamute, Basset Hound, Beagle, Border Collie, Boston Terrier, Bouvier Des Flandres, Cairn Terrier, Cardigan Welsh Corgi, Chihuahua, Dachshund, Cocker Spaniel, Giant Schnauzer, Great Dane, Maltese Terrier, Manchester Terrier, Miniature Pincher, Norfolk Terrier, Norwegian Elkhound, Norwich Terrier, Saluki, Poodle, Pembroke Welsh Corgi, Samoyed, Scottish Terrier, Shih Tzu, Siberian Husky, Wire-Haired Fox Terrier, Tibetan Terrier, West Highland White Terrier, Whippet, Smooth-Coated Fox Terrier.
Persians and Siamese.
The cost is £22.98 for a measurement, either added to a consult with the vet when being seen for a non opthalmology case or specific eye case. Alternatively a nurse appointment can be made to check a susceptible breed with one of our skilled nurses. Contact the surgery and arrange a check.
STRESS
Our pets can suffer various forms of stress like ourselves. The use of pheromones can help alleviate many forms of stress. Adaptil and Feliway are 2 range of products that can help tremendously.
Below is some information about the products and some videos to download and watch. All the products are available from reception.
Now there is a new Feliway product to prevent cats scratching the furniture!
COLOUR CODES ON GUIDE DOG HARNESS

The Guide Dog on the left has a red and white flash on its harness, signifying that the guide dog owner has hearing loss as well as a visual impairment.
The guide Dog on the right has a blue and white flash on its harness, signifying that the guide dog owner suffers from seizures, as well as visual impairment, and the dog is also a seizure alert dog.
BABY WILD BIRDS
Finding a wild baby bird that is unable to fly well when out walking is not an uncommon event. The first impulse may be to help the young bird, but in the majority of cases the young bird does not need help. In fact, interveining often makes the situation worse.
Here is how to determine whether to take action:-
The first thing to do is to ascertain if the baby bird is a nestling or a fledgling.

Nestling (left) and Fledgling (right)
Most of the baby birds people find are fledglings. These are young birds that have just left the nest, are still under the care of their parents, and do not need our help. Fledglings are feathered and capable of hopping or flitting, with toes that can tightly grip your finger or a twig. These youngsters are generally adorable and fluffy, with a tiny stub of a tail.
When fledglings leave their nest they rarely return, so even if you see the nest it's not a good idea to put the bird back in, as it will most likely hop back out. Usually there is no reason to intervene at all beyond putting the bird on a nearby perch, out of harm's way and keeping pets indoors, if it is in your garden. The parents may be attending to 4 or 5 young scattered in different directions, but they will return to care for the one you have found. You can watch from a good distance to make sure the parents are returning to care for the fledgling.
If the baby bird is sparsely feathered and not capable of hopping, walking, flitting or gripping tightly to your finger, it's a nestling. If so. the nest is almost certainly nearby. If you can find the nest (it may be well hidden), put the bird back as quickly as possible. Don't worry parent birds do not recognise their young by smell! They will not abandon a baby if it has been touched by humans.
If you have found both parents dead, the young bird is injured, you can't find the nest (remember this can be difficult, so search hard), or are absolutely certain that the bird was orphaned, then contact a wildlife rehabilitator, like the RSPCA or a vet.
Remember that the vast majority of "abandoned" baby birds are perfectly healthy fledglings whose parents are nearby and watching out for them.
LILIES toxic to cats
With Easter approaching, please remember that Lilies are toxic to cats. Take care to avoid the Easter Lily, Tiger Lily, Rubrum Lily, Stargazer Lily, Japanese Show Lily, Asiatic Lilies and species of the Day Lily. However, it is wise to be cautious with all types of lily. Any part of the plant is dangerous, including the pollen and flower.
Other plants that are potentially poisonous to cats are:-
Azalea, Oleander, Sago palm, Yew plant.
Cat owners should also be wary of Cyclamen, Poinsettia, Amaryllis, Holly, Ivy, Mistletoe, Daffodils and Foxgloves.
Laburnum, some berries and toadstools can also occasionally cause problems.
Remember cats are inquisative and can accidentally eat parts of plants.

POTENTIAL POISONS FOR YOUR DOG

If you are worried about the ingestion of any of these then contact the surgery immediately.

Link to Poisonous plants website:-
BUNNY DENTIST
Dental disease in pet rabbits is one of the commonest problems we see. Rabbits have constantly growing teeth and require daily wear to keep the teeth normal. Signs of dental problems can include excessive salivation and drooling around the chin, loss of appetite (in the early stages selective eating is seen, avoiding hard foods) , tooth grinding due to pain, dullness, and gut problems.
Rabbits in the wild exist on a meagre diet that is mainly fibre / roughage. In domestication, we have provided a carbohydrate rich diet and as a result reduced fibre. Rabbits are selective eaters, and given the choice will eat the wrong things. It is important we provide the right diet for good dentition, and this is a mainly fibre diet with fresh vegetables in moderation and a SMALL portion of rabbit pellets (not the museli style rabbit mix) daily. A specific rabbit pellet is preferable. Rabbits also need daily exposure to ultraviolet from daylight for good bone formation to allow a solid base for the teeth.
it is a good idea to check your rabbit for signs of dental disease, drooling or malaligned / overgrown incisors (see normal rabbit below). If there are signs of dental disease, especially if this is coupled with a poor appetite then arrange for us to check your pet, where we can inspect the back molars with a scope. If you are not sure what to look for then let us show you!
Remember rabbits are very good at hiding signs of pain.
We can email you, on request, a link to a page on our website to download our Rabbit Booklet

SIGNS YOUR RABBIT IS UNWELL
Rabbits can hide signs of illness and make it difficult to spot when they are unwell.

RABBIT HEALTH
Information on Rabbits
CLICK ON EACH IMAGE TO ENLARGE AND READ
HIDDEN RISK OF HORSE MANURE TO DOGS !!
Dogs eating horse manure could be poisoned by insecticide contained within it. Horses in the UK are generally wormed once or twice a year, and most owners will worm them just before the grass starts to grow in February/March.
Most horse wormers contain Ivermectin which can cause serious illness in dogs, but could be fatal to collies. Most dogs will be drawn to fresh horse manure, although ivermectin within the manure can remain active for some time. Initial symptoms may be dilated pupils, an unsteady gait or possible seizures, difficulty breathing, or in severe cases coma. Once absorbed the toxic effect cannot be reversed, but if a dog has just (within 4-6 hours) eaten horse manure and there is a risk of toxicity then it could be given an emetic (a drug to induce vomiting) to help it vomit the ingesta. Treatment of cases of toxicity involves fluid therapy, intensive care, and medication to control seizures. Prognosis is guarded.
Symptoms may not be apparent immediately, it depends on how fresh the manure is and how much was eaten. It could take weeks for ill effects to show.
Levels of ivermectin are strong in horse/sheep/cow poo for 3-4 days after dosing with ivermectin wormers. The levels break down rapidly in sunlight. it can decrease to low levels by 14 days after dosing in horses and sheep, and 21 days in cattle.
CHOCOLATE POISONING

Chocolate - A Timely Reminder
Chocolate poisoning in dogs continues to be amongst the most common enquiries we receive each year. With Easter approaching, it must be remembered that chocolate-based treats and gifts can be toxic to our pets.
Chocolate is made from cocoa beans, the dried and partially fermented seeds of Theobroma cacao native to the deep tropical region of Central America. The toxic constituent, theobromine, is a methylated xanthine. Chocolate also contains a small amount of caffeine.
The amount of theobromine in chocolate products varies considerably due to natural differences in cocoa beans as well as the ingredients of products. There may also be some genetic susceptibility to theobromine toxicity in certain breeds. White chocolate is very low in theobromine and therefore considered non-toxic.
In dogs, the most common clinical signs include vomiting, abdominal discomfort, diarrhoea, polyuria (excessive drinking) and bloating. Theobromine intoxication will also stimulate the myocardium (heart muscle) and central nervous system stimulation - resulting in tremors, tachycardia (fast heart rate) and hyperthermia. There is also the risk of pancreatitis following ingestion of chocolate products that contain a large amount of sugar and fat.
Treatment is largely supportive with particular emphasis on the management of cardiovascular and neurological effects, as well as rehydration. The prognosis is generally good and most dogs make a full recovery within 48-72 hours. There have been very few fatal cases reported (about 5 in 1000).
As a rough guideline, levels of Theobromine at 20mg/kg body weight are toxic, 40-50mg/kg cause severe signs, and 60mg/kg can cause seizures.
So as a guide ingestion of more than 3.5 grammes of Dark Chocolate / kg body weight should seek treatment. For Milk Chocolate ingestion of more than 14 grammes / kg should seek treatment and generally white chocolate is not regarded as toxic.
Chocolate is also toxic to cats, rodents and rabbits, but there are limited case reports, therefore a treatment dose is yet to be established. Cats seem less inclined to eat chocolate, although each year there are a few cases where significant clinical effects are seen.
BABESIOSIS AND TICKS
 New tick-borne disease in dogs, canine babesiosis, found in the UK
New tick-borne disease in dogs, canine babesiosis, found in the UK
Scientists at University of Bristol conducting the Big Tick Project say recent confirmed cases of Babesia canis in four dogs in Essex that had not travelled abroad, have increased the need for surveillance of tick-borne disease in the UK.
Launched last year, the Big Tick Project has become the largest-ever veterinary study of ticks and tick-borne disease in the UK, if not worldwide. In addition to the potential for tick mapping and greater understanding about what is perceived to be a rise in the risks to dogs and people from Lyme Disease, the emergence in four dogs in Essex of babesiosis, a life-threatening disease transmitted to dogs by infected ticks usually found in Europe, has highlighted the need for a major investigation on the scale of the Big Tick Project, says Professor Wall. Professor Wall says: “The recent Babesia cases in Essex are of huge significance. The fact that we now appear to have established populations of the tick Dermacentor reticulatus acting as vectors of the introduced pathogen Babesia canis is a new and important development and a major concern for animal health. It clearly demonstrates the potential dangers from the inadvertent introduction of novel disease pathogens if vigilance and surveillance are not maintained.”
 Dog owner Hollie Wilson’s dream French holiday with husband Craig and two dogs Olive and Badger turned into a nightmare when Olive, a pointer, was bitten by a tick. Within days, Olive’s condition had deteriorated and it was clear that she was becoming seriously unwell. On arrival back in the UK, the Wilson’s rushed their dog to their vet and after extensive tests, canine babesiosis, suspected by the vet on duty that day who had seen the disease in her native Poland, was confirmed.
Dog owner Hollie Wilson’s dream French holiday with husband Craig and two dogs Olive and Badger turned into a nightmare when Olive, a pointer, was bitten by a tick. Within days, Olive’s condition had deteriorated and it was clear that she was becoming seriously unwell. On arrival back in the UK, the Wilson’s rushed their dog to their vet and after extensive tests, canine babesiosis, suspected by the vet on duty that day who had seen the disease in her native Poland, was confirmed.
Hollie says: “Her gums were completely white and she was anaemic. The race was on to find the recommended drug treatment and there was a lot of ringing round before she could finally be treated.
“I can honestly say without all the help from our vets, Olive would not be here today. It was due to their persistence in finding she had babesiosis and how Olive was treated so quickly, that she has made a full recovery.
“Looking back, losing Olive to babesiosis would have been heart-breaking.
“Back then, I probably wasn't aware so much of the risks of tick-borne disease before all this happened and was probably a bit naive as to where these risks were found. However I am most definitely aware of the dangers carried by ticks now!
“I think my message is to talk to your vet and find a tick treatment that is effective for your dog and ensure you use it on a regular basis as you never know which tick is infected. Although Lyme disease is well documented I am all too well aware now of the risk of other diseases that can be life threatening such as babesiosis. Seeing the disease being carried in ticks in the UK is extremely worryingly as a dog owner and more needs to be done through campaigns such as The Big Tick Project to raise awareness.”
 What are the symptoms of Babesia Canis?
What are the symptoms of Babesia Canis?
Symptoms of babesiosis can range from mild to severe and include lethargy, lack of appetite, fever, anaemia, pale gums, an enlarged abdomen, weight loss and jaundice. If your dog has or had ticks and you are concerned for the health of your dog, please contact a vet immediately.
Detecting ticks
Check your pets’s skin on its head first (around the mouth and ears, behind ears and on its neck), then work your way down its forelegs and the rest of its body, searching for any lumps on the skin surface.
If you find a lump:
• Part the hair and look at it more closely (with the help of a magnifying glass, if necessary)
• The place where the tick attaches may or may not be painful and there may be skin swelling - It is distinguished from other skin swellings and growths because close scrutiny can reveal the tick’s legs at the level of the skin.
What to do if you find a tick
When attempting to remove a tick avoid handling the parasite directly. Wear gloves and dispose of ticks hygienically so they cannot re-attach themselves or lay eggs.
If you find a tick on your pet’s skin:
• The aim is to remove the whole tick, including its mouthparts without squeezing the tick's body
• Use a specially designed hook or scoop with a narrow slot that traps the tick's mouthparts
• Slide the hook under the tick at skin level so as to grip the head of the tick, ensure that the hook is not entangled
• Scoop out the tick – rotating the hook around the tick's head may help dislodge the mouthparts before removal
• Flush the tick down the lavatory (or sink - with hot water)
Do not attempt to burn, cut or pull the tick off with your fingers
- Buy a tick removal tool and keep it in your pet first-aid box
- If in doubt, take your pet to the vet
How to protect your dog from Ticks and tick borne disease
To reduce the risk associated with ticks on dogs, veterinary surgeons have innovative and convenient treatments that are only available on prescription. The options available to protect dogs against ticks include spot-ons , sprays, collars and oral chewable formulations. For best advice on how to remove a tick correctly from your pet please speak to your vet.
For more information please contact us .
TICK ALERT
Scientists have said climate change is likely the cause for the increase in tick numbers in the UK. More worrying is the appearance of a continental tick called Dermacentor Reticularis,

normally not identified here, and can transmit serious illnesses like babesiosis, ehrlichiosis and also lyme disease which is already spread by our UK tick Ixodes Ricinus. These diseases can affect many types of pets, and people. Good tick control on our pets has become so important. We have effective tick treatments, including a tablet lasting 3 mths!!
ALABAMA ROT
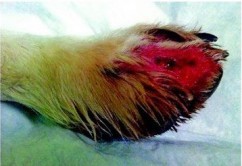
A dog was confirmed as dying from Alabama rot in Moberley, Cheshire (2016). While this is a serious disease, it still remains relatively uncommon. Symptoms include well demarcated ulcerative skin lesions, mainly on the lower limbs and paws, but can be seen on the head, and some lesions have been reported on the tongue. Shortly after the appearance of these lesions the affected dogs can progress to kidney failure, with symptoms including vomiting, reduced appetite, lethargy and excess drinking.
The cause of Alabama rot or Cutaneous and Renal Glomerular Vasculopathy (CRGV) is still unknown, although research is underway to identify the cause. Lesions are as a result of developing microthrombi that block blood vessels. It is important should you suspect a case, to arrange a veterinary examination, where tests may be indicated.
JERKY TREATS health risk

WARNING!
Recently we have seen a syndrome associated with the feeding of Jerky dog treats. They have been dried 'jerky' type dog treats (chicken and duck), of which many have been identified as originating from China. Symptoms are as a result of developing kidney disease, with excess thirst and urinating, poor appetite and glucose in the urine but no raised glucose in the blood. The disease is caused by damage to the sensitive tubules in the kidney.
Our current advice is not to feed these treats.
CANCER THERAPY - The Future
Ground breaking work at Cambridge University and the University of Southampton could hold a future therapy for cancer in people and animals. They are trying to make the natural killer T cells that are in our bodies target specific cancer cells. This would allow our own bodies to eliminate cancer cells when they develop. Below are 2 great videos explaining how these cells work:-
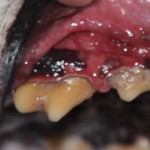
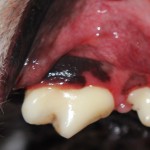
DENTAL DISEASE
Pets suffer from dental disease like we do, but sadly they can't tell us their mouths are sore. Many dogs and cats adapt to painful mouths and carry on trying to eat. Despite eating, each meal results in painful moments. Another effect of poor teeth is the development of bad breath which we can detect. Anyone who has had a tooth ache will tell you it affects their day to day chores.
How often should we check pets mouths? Ideally check dogs and cats mouths at least weekly for any pain or smell. If any abnormalities are detected then it is advisable to book a consultation to check their teeth..
When dental disease is detected, diseased teeth can be removed and the remaining teeth descaled under a general anaesthetic. At the post dental check up, it is amazing how much happier they are, and their owners remark they had not realised their pets had not been well for so long.
Dental disease can also affect pets internal health, with effects on the heart, kidneys, liver and other organs.
Ideally cleaning our pets teeth can prevent dental disease. Cleaning teeth daily is the goal, but doing so 2-3 times per week is better then not doing it. Pet specific toothpaste with poultry or beef flavouring is recommended.
LOOK (inspect their teeth), SMELL (sniff their breath) and OBSERVE (watch them eating)
BOOK A DENTAL CHECK TODAY
SLUGS AND SLUG PELLET POISONING
 The recent wet and humid weather has created perfect conditions for slugs, increasing the likelihood of dogs coming across them. This increases the risk of ingesting slugs that have been exposed to slug bait molluscicide agents.
The recent wet and humid weather has created perfect conditions for slugs, increasing the likelihood of dogs coming across them. This increases the risk of ingesting slugs that have been exposed to slug bait molluscicide agents.
Slugs transmit lungworms to dogs when they are eaten. This can cause a serious and often fatal haemorrhagic lung disease in dogs. If your dog eats slugs or snails, or chews grass that may have slugs on it, then regular worming is advised. Prevention is by using a wormer effective against lungworm monthly (we can advise on appropriate wormers).
Ingestion of a non infected slugs can typically result in mild clinical signs of vomiting, diarrhoea, abdominal discomfort and hypersalivation, requiring minimal treatment, if any. However if the slugs have ingested or been killed by slug pellets, and dogs have eaten several of them, then they are at risk of poisoning. Metaldehyde, which is a common molluscicide, has an extremely low toxic dose and the ingestion of a relatively small amount of either the bait itself or poisoned slugs can be potentially fatal to dogs, causing gastrointestinal signs as well as rapid-onset tremors, twitching and convulsions. Ingestion of slug bait containing metaldehyde represents one of the biggest causes of poisoning fatalities in dogs.
Pet friendly slug baits are available from garden centres, so read the label and avoid any containing metaldehyde specifically.
ALLERGIC SKIN DISEASE EXPLAINED
 Allergic skin disease is one of the commonest causes of skin problems in dogs. Currently we believe that individuals that are more prone to allergies have a genetic abnormality in their white cell (defence cells) function that does not suppress the normal role of the body in protecting against infections. As a result when a harmless invader, e.g. pollen, is met by the body, it over reacts causing inflammation at the site of contact.
Allergic skin disease is one of the commonest causes of skin problems in dogs. Currently we believe that individuals that are more prone to allergies have a genetic abnormality in their white cell (defence cells) function that does not suppress the normal role of the body in protecting against infections. As a result when a harmless invader, e.g. pollen, is met by the body, it over reacts causing inflammation at the site of contact.
Special cells called langerhan cells capture the allergen, e.g. pollen or dust mite, from the skin surface and present it to the defence cells. Suppressor cells should dampen the response to such harmless invaders, and no symptoms develop. In allergic dogs this does not happen and the full might of the immune system is unleashed. The result is inflammation and redness at the point of entry, which in dogs is usually face, eyelids, muzzle, armpits, groin and feet. Damage to the skin then results in secondary infections. Seasonality of symptoms will relate to the respective allergens occurrence.
It is usual for a period of time to be needed for the body to become sensitised to the offending allergen, so symptoms in dogs commonly start between 1-3 years of age. Initially these can be very mild and often overlooked, but with time they will progress. Most owners become very frustrated that the allergy is recurrent, but it is important to realise, once an allergy develops, it will be LIFE LONG. The goal is to design an effective control regime for a dog’s life to keep symptoms at bay.
Certain breeds seem more prone to allergies than others. Most cases of allergies will worsen if secondary infections with bacteria or yeasts develop, or they become infested with fleas.
Uncomplicated allergies can be controlled with a variety of treatments and each individual will respond uniquely to combinations. Treatments range from steroids to immunotherapy, including antihistamines, immunosuppresants and some new targeted drugs preventing itch. Control of any infections is very important.
Where indicated, it is possible to perform skin testing to explore which allergens are involved. The test kits have a limited number of allergens, the commonest ones seen, so unusual allergens will not be detected. Identifying the allergen does not necessarily mean that it can be avoided, e.g. housedust mite which is ubiquitous in our houses. The main reason to skin test is to explore the possibility of using immunotherapy as a therapy, where incremental small doses of the substance causing the allergy are injected over time to desensitise the individual. Success with this therapy varies but can be about 60-70% but does take time to develop.
So why are we seeing more allergies in people and pets. The truth is we do not know the definitive answer, but one interesting theory is that people and pets are being exposed to less parasites and infections, which would usually occupy the immune system. As a result the immune system is directed against harmless invaders.
DOG FAECES RISK TO LIVESTOCK
“Do I need to pick up my dog poo on farmers land?”
The short answer is "yes", .......read on.
 There is growing evidence of the links between two specific diseases in livestock and the presence on grazing land of faeces from infected dogs. The two diseases are NEOSPOROSIS, which can cause abortion in cattle, and SARCOCYSTOSIS, which can cause neurological disease and death in sheep.
There is growing evidence of the links between two specific diseases in livestock and the presence on grazing land of faeces from infected dogs. The two diseases are NEOSPOROSIS, which can cause abortion in cattle, and SARCOCYSTOSIS, which can cause neurological disease and death in sheep.
Neosporosis is caused by the parasite Neospora caninum, whose eggs are present in infected dog’s faeces. Dogs are the natural host and studies have shown that subclinical infection can occur, showing no outward signs of disease. There is a higher incidence in dogs being fed raw diets.
Pasture or water contaminated with neospora will allow ingestion by cattle. Studies have shown that infection in cattle is common, but can result in disease with abortion a common sign. There are currently no drugs or vaccines to prevent this in cattle.
Sarcocystosis is caused by the parasite Sarcocystis sp., which has a number of intermediate hosts, including dogs. Spread is by contaminated dog faeces on pasture. Heavy infections in sheep can result in symptoms, but even in symptomless cases, the present of cysts of the parasite in the carcase in the food chain will result in it being condemned. At present there is no vaccine, and treatment is prohibitively expensive.
What can be done?
As responsible pet owners we should pick up dog faeces after our pets have messed on farmers land. The farmers have kindly allowed access to their land so we should respect their livelihood. Raw meat diets are potential sources of infection, so consider changing. If this is not possible then the risk can be reduced but not eliminated by freezing the food for a few days before feeding it.
PICK UP DOG POO!!!